What is Cognitive Behavioural Therapy for Social Anxiety?
Cognitive Behavioural Therapy, commonly referred to as CBT, is an umbrella term for therapies based on cognitive and behavioural theories of psychotherapy. Some of these CBT therapies are recommended for people with social anxiety.
The NHS offers CBT as part of its Talking therapies program. Different mental health services cover the provision in Scotland and Wales. The principles of CBT are also applied in other therapy scenarios – including self-help.
 So, what is CBT and how does it work?
So, what is CBT and how does it work?
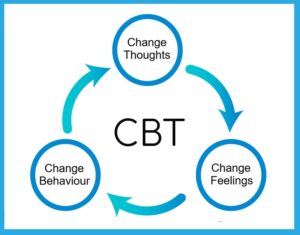
C stands for cognition (thought), B (behaviour), T (therapy). CBT is based on the idea that your thoughts, feelings, physical sensations and behaviour are all interconnected.
For example, we’re speaking to a friend (situation) and we may worry about how we are behaving or sound (thoughts). At the same time, we may feel anxious (emotion) and then experience sensations such as feeling shaky or have a dry mouth (physiological symptoms). We may keep quiet, play safe, or leave the situation (behaviours). Afterwards, we may worry even more about how we well we did, how we felt inside, what the friend may now think of us, and the cycle continues.
The central idea in CBT is that by applying techniques to change your thinking and behaviour you can break the cycle that keeps the anxiety going. See our page on the social anxiety maintenance cycle.
CBT is sometimes referred to as having a ‘here and now’ focus, unlike some other therapies. CBT will take into account of your past, but sessions tend to be focused on the present-day difficulties.
What Should I Expect from therapist-led CBT?
CBT for social anxiety has several main elements:
- Assessment and formulation: A formulation is a diagram that helps the therapist and client come to a shared understanding about how a person’s focus of attention, thoughts, emotions, physiological symptoms, behaviours, and life experiences contribute to their difficulties today.
- Psychoeducation: The therapist helps you understand social anxiety, how that anxiety impacts you physiologically, and the role of focus of attention, thoughts, physiological symptoms, and avoidance and safety behaviours.
- Active therapy: Rather than just talking about difficulties to gain insight into them, CBT will involve active tasks to do in session and out of session as homework to work on those difficulties.
- Skills development: An important part of CBT is to learn a set of therapeutic techniques that can be applied over time to benefit the person beyond their therapy sessions.
- Regularity: regular and consistent practice is one of the most important factors in using CBT. This can be difficult, as it may initially increase anxiety. Maintaining the motivation to confront feared situations, even when some may not go well, is key.
- Structured and goal focused: CBT is a highly structured and goal focused therapy. Sessions will likely include regular reviews and agenda setting.
NHS CBT for social anxiety is recommended to be offered on a one-to-one basis but can sometimes be delivered in a group. One-to-one sessions are typically 12-16 sessions of 60-90 minutes each with a trained NHS Talking Therapist. The exact number of sessions and their length can vary depending on need and your local Talking therapy service. Sessions can be face-to-face or remote via an online video call. Both the type of support available and how you access it will depend on local availability.
Why CBT for Social Anxiety?
CBT is considered to be the frontline evidence-based treatment for social anxiety. The UK National Institute for Health and Care Excellence (NICE) have surveyed and reviewed the efficacy and effectiveness of different treatments for mental health conditions and made recommendations for what should be made available in the NHS, which includes CBT for social anxiety. See NICE guidance for social anxiety.
Figures on CBT social anxiety recovery rates vary and recovery can be hard to define and therefore measure. However, based on the research currently available, and how they measure recovery, CBT has the largest evidence base for both recovery and improvement.
An analysis of the available research in 2022 showed moderate to large improvements in long-term social anxiety symptoms with therapist assisted CBT compared to no treatment. This shows that the improvements tend to last. Studies showing long-term recovery like this helped lead to the NICE guidance recommending CBT for people with social anxiety.
Real world recovery outcomes can vary between service providers but still show a lot of people making progress.
There is no limit to the number of times you can do NHS CBT but some NHS regions may have restrictions such as requiring a delay in re-referral. Some people find one course is enough, and others need more. Each time, it can be a different experience, based on many factors. If CBT has not been helpful before, it does not mean it may not help again.
NICE periodically updates its recommendations and is a useful resource providing an overview of treatment options.
Not everyone finds CBT to be helpful. If you feel CBT is not for you, the NICE guidelines also include alternative treatment options – depending on local availability – see Other NHS treatment options
Research is continually being produced and other therapies show promise, but many more studies are needed. Examples include Acceptance and Commitment Therapy (ACT), Eye Movement Desensitisation and Reprocessing Therapy (EMDR), Emotion Focused Therapy (EFT), and Compassion Focused Therapy (CFT).
CBT protocols and interventions
On the recommendation of NICE, NHS CBT follows evidence-based protocols for social anxiety. Although there are these guiding protocols for treating social anxiety, every client and therapist are different, and the therapy is tailored to the specific client’s needs.
Some therapists may bring in other techniques that they think are helpful for your specific situation. What works for you may not work for someone else with social anxiety, and vice versa.
Changing what we do or how we think is often a powerful way to improve how we feel and our quality of life. It is important to remember change can take time and practice. It is rarely as simple as just one or two techniques or changes to behaviour. There is a process, and that can often take time. This is why CBT equips individuals with a range of practical tools and techniques they can use independently to manage their emotions and behaviours even after therapy ends.
Common techniques that a CBT therapist might use in the treatment of social anxiety include:
- Reducing Avoidance and Safety Behaviours
- Challenging unhelpful thought patterns
- Retraining your Focus of attention
- Behavioural experiments and exposure hierarchies
You can try some of these techniques out for yourself as part of your CBT therapy.
NHS Guided self-help
Some NHS regions may also offer ‘guided self-help’ but this will generally be for mild and moderate cases. This is when some professional support is included (for example, brief check-ins with a practitioner) with self-help information. It requires consistent motivation to practise regularly and apply the techniques consistently. While it may not be suitable for everyone, especially those with more severe difficulties, guided self-help can be an accessible first step for some.
What about self-help CBT?
The NHS social anxiety webpage states “self-help can help reduce social anxiety and you might find it a useful first step before trying other treatments”. Although therapist led NHS Talking Therapy (via CBT) is the key recommendation, self-help CBT approaches can be useful if you are not yet ready to see a therapist, are on a waiting list, or you prefer to start working on your social anxiety at your own pace. See our pages on self-help.
How to access CBT?
You can access talking therapies, including CBT, through the NHS. You can usually refer yourself directly to your local talking therapy service without a referral from your GP. Alternatively, your GP can refer.
You will then be offered an opportunity to speak with a clinician about your difficulties and consider what treatment and/or service would be best suited to support you and your current needs. The NHS NICE guidance recognises that attending a doctor’s appointment – or talking to a clinician – can be very difficult for those with social anxiety. It provides a series of recommendations to make communication and appointments easier. You may be able to ask your GP to ring you rather than you having to attend the GP practice in person. You could ask friends or family to help you make the first phone call. You could ask your health and social care team to communicate with you over text or email.
You can also self-refer – find details of your local NHS Talking Therapies service here.
Different areas often have different service providers and policies, and the waiting times might vary. This might mean you want to choose a different way to access therapy, and you might want to work with a therapist privately, self-funded or through a health insurance policy.
If you are going to work with a private therapist, it is important to find the right one. In the UK, ‘therapist’ is not a protected title which means anyone can call themself a therapist. We recommend checking if they are ‘accredited’, which means they are governed by a professional body (in the UK, this is BABCP for CBT therapists). More information is included on our pages on finding a private therapist.
Common Misconceptions
The idea of simply changing our thoughts might suggest CBT is a simplistic therapy.
“It’s just positive thinking”.
CBT is not simply learning to think more positively. It involves identifying and changing unhelpful thinking patterns into more realistic and balanced thoughts to see if there are other ways to view ourselves or situations. It’s not about ignoring problems but addressing them in a constructive way.
“NHS CBT is too short, I can’t fix all my problems in this time”.
When we have been experiencing our difficulties for a long time, we can often feel like a short-term intervention is not enough support. While CBT is often more short-term compared to some other therapies, it’s not an overnight solution. It requires commitment and practice over time to see lasting results.
“It ignores the past”.
CBT does focus on ‘the here and the now’. It looks at how thoughts and behaviours in the present maintain the effects of the past. This can include exploring how past experiences influence current thought patterns, but the emphasis remains on the present and future.
“It’s too structured and rigid”.
While NHS CBT (via therapist-led Talking therapy) has a structured framework, it’s not overly rigid. Although there are guiding protocols for treating social anxiety, every client and therapist are different, and the therapy is tailored to the specific client’s needs.
Conclusion and Links
For further exploration and a deeper understanding of CBT:
NHS website: Overview – Cognitive behavioural therapy (CBT)
NHS website: How it works – Cognitive behavioural therapy (CBT)
British Association for Behavioural and Cognitive Psychotherapies (BABCP) website: What-is-CBT
MIND provide valuable insights into the nature and practice of CBT including video: Cognitive behavioural therapy (CBT)
References
Kennerley, H., Kirk, J., & Westbrook, D. (2016). An introduction to cognitive behaviour therapy (3rd ed.). SAGE Publications.
Overview: Social anxiety disorder: Recognition, assessment and treatment: Guidance. NICE. (2013, May 22). https://www.nice.org.uk/guidance/cg159
Roth, A., & Fonagy, P. (2005). What works for whom: A critical review of psychotherapy research (2nd ed.). Guilford Publications.
Butler, Gillian (1999). Overcoming Social Anxiety and Shyness: A Self-Help Guide Using Cognitive Behavioural Techniques. London: Constable & Robinson Ltd.
National Institute for Health and Care Excellence (NICE), Social anxiety disorder: recognition, assessment and treatment, Full Guidance, Section 6.11.2


